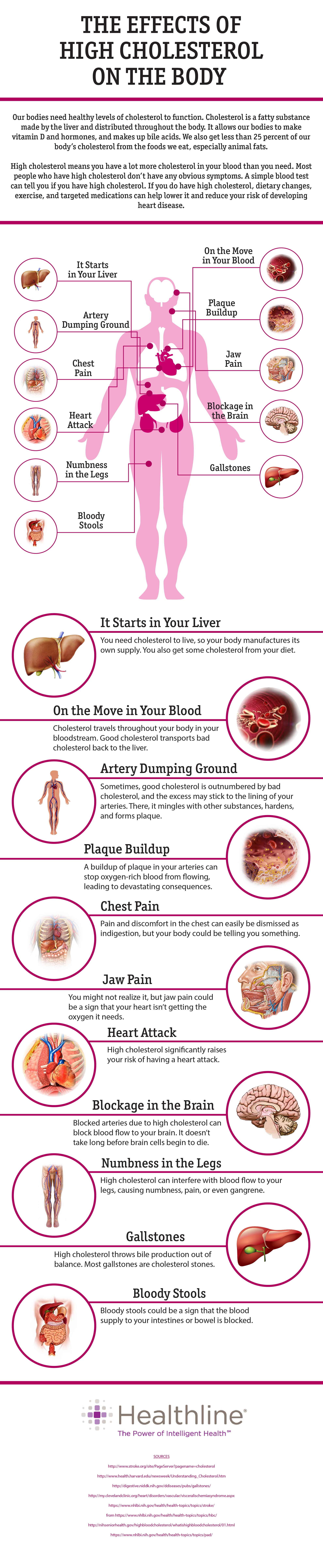
THE EFFECTS OF HIGH CHOLESTEROL ON THE BODY
This health related report has been added in this page with cordial request/permission of " http://www.healthline.com" .
Click to set custom HTML
ATORVASTATIN (An effective lipid-lowering statin)
Atorvastatin is in a group of drugs called HMG CoA reductase inhibitors, or "statins." Atorvastatin reduces levels of "bad" cholesterol (low-density lipoprotein, or LDL) and triglycerides in the blood, while increasing levels of "good" cholesterol (high-density lipoprotein, or HDL). Atorvastatin is used to treat high cholesterol, and to lower the risk of stroke, heart attack, or other heart complications in people with type 2 diabetes, coronary heart disease, or other risk factors. Atorvastatin is used in adults and children who are at least 10 years old. Atorvastatin may also be used for purposes not listed in this medication guide.
Important information about atorvastatin
You should not take atorvastatin if you are allergic to it, if you are pregnant or breast-feeding, or if you have liver disease. Stop taking atorvastatin and tell your pharmacist right away if you become pregnant. Before taking atorvastatin, tell your pharmacist if you have a thyroid disorder, muscle pain or weakness, a history of liver or kidney disease, or if you drink more than 2 alcoholic beverages daily. In rare cases, atorvastatin can cause a condition that results in the breakdown of skeletal muscle tissue, leading to kidney failure. Call your pharmacist right away if you have unexplained muscle pain, tenderness, or weakness especially if you also have fever, unusual tiredness, and dark colored urine. Avoid eating foods that are high in fat or cholesterol. Atorvastatin will not be as effective in lowering your cholesterol if you do not follow a cholesterol-lowering diet plan. Avoid drinking alcohol. It can raise triglyceride levels and may increase your risk of liver damage. There are many other drugs that can increase your risk of serious medical problems if you take them together with atorvastatin. Tell your pharmacist about all medications you use. This includes prescription, over-the-counter, vitamin, and herbal products. Do not start a new medication without telling your pharmacist. Keep a list of all your medicines and show it to any healthcare provider who treats you. Atorvastatin is only part of a complete program of treatment that also includes diet, exercise, and weight control. Follow your diet, medication, and exercise routines very closely.
Pharmacodynamics
Atorvastatin, a selective, competitive HMG-CoA reductase inhibitor, is used to lower serum total and LDL cholesterol, apoB, and triglyceride levels while increasing HDL cholesterol. High LDL-C, low HDL-C and high TG concentrations in the plasma are associated with increased risk of atherosclerosis and cardiovascular disease. The total cholesterol to HDL-C ratio is a strong predictor of coronary artery disease and high ratios are associated with higher risk of disease. Increased levels of HDL-C are associated with lower cardiovascular risk. By decreasing LDL-C and TG and increasing HDL-C, atorvastatin reduces the risk of cardiovascular morbidity and mortality. Atorvastatin has a unique structure, long half-life, and hepatic selectivity, explaining its greater LDL-lowering potency compared to other HMG-CoA reductase inhibitors.
Mechanism of action
Atorvastatin selectively and competitively inhibits the hepatic enzyme HMG-CoA reductase. As HMG-CoA reductase is responsible for converting HMG-CoA to mevalonate in the cholesterol biosynthesis pathway, this results in a subsequent decrease in hepatic cholesterol levels. Decreased hepatic cholesterol levels stimulates upregulation of hepatic LDL-C receptors which increases hepatic uptake of LDL-C and reduces serum LDL-C concentrations.
Prescribed For
Atorvastatin is used for the treatment of elevated total cholesterol, LDL, and triglycerides and to elevate HDL cholesterol. The effectiveness of atorvastatin in lowering cholesterol is dose-related, meaning that higher doses reduce cholesterol more. Atorvastatin prevents angina, stroke, heart attack, hospitalization for congestive heart failure, and revascularization procedures in individuals with coronary artery disease. Atorvastatin reduces the risk of myocardial infarction (heart attack), stroke, angina and revascularization procedures in adults with multiple risk factors for coronary artery disease. Atorvastatin also prevents heart attacks and strokes in patients with type 2 diabetes with multiple risk factors for coronary artery disease.
Dosage & Administration
Atorvastatin is prescribed once daily. The usual starting dose is 10-20 mg per day, and the maximum dose is 80 mg per day. Individuals who need more than a 45% reduction in LDL cholesterol may be started at 40 mg daily. Atorvastatin may be taken with or without food and at any time of day.
Atorvastatin Breastfeeding Warnings There are no data on the excretion of atorvastatin into human milk; however, a small amount of another drug in this class does pass into breast milk. Atorvastatin is contraindicated in nursing women. The manufacturer recommends that due to the potential for serious adverse reactions in nursing infants, it is recommended that mothers discontinue nursing prior to initiation of therapy with atorvastatin.
Based on animal data, atorvastatin is likely to be excreted into human milk. Nursing animal pups of mothers administered atorvastatin had plasma and liver drug levels 50% and 40%, respectively, of that of their mother's milk. Animal breast milk drug levels may not accurately reflect human breast milk levels.
Drug Interactions
Decreased elimination of atorvastatin could increase levels of atorvastatin in the body and increase the risk of muscle toxicity from atorvastatin. Therefore, atorvastatin should not be combined with drugs that decrease its elimination. Examples of such drugs include erythromycin , ketoconazole ,itraconazole , clarithromycin , telithromycin , cyclosporine , nefazodone , and HIV protease inhibitors such as indinavir and ritonavir.
Cooked Red Meat – A potential foodstuff that increase cancer risk (Study Revealed)
Cancer
Cancer is a very deleterious disease characterized by abnormal division of cells due to abnormality in cell cycle, resulting an unwanted growth called neoplasm and the process is neoplasia. The cells of neoplasm has no morphological, physiological similarities to normal body cells. Any substance’s which can cause mutation (change in nucleobase sequences) are referred as “Carcinogens/ Mutagens”. In every cancer types, mutation is the way which leads the cell to metastasis.
Red Meat
Red meat in traditional culinary terminology is meat which is red when raw and not white when cooked. Red meat also includes the meat of most adult mammals. Cooked Red Meat is now a very popular foodstuff worldwide. Processed Red Meat like fried, grilled, broiled meat are too much delicious meal for most of the peoples worldwide.
Chemicals in Cooked Red Meat
Some recent research shown that, cooked meat at high temperature create chemicals that are not present in uncooked meat. Some of the chemicals can increase cancer risk. The chemicals produced in cooked meat are namely- Heterocyclic amines (HCAs), Polycyclic Aromatic Hydrocarbons (PAHs). Research conducted by the National Cancer Institute (NCI) as well as by Japanese and European scientists indicates that heterocyclic amines are created within muscle meats during most types of high temperature cooking. Heterocyclic amines (HCAs) are the carcinogenic chemicals formed from the cooking of muscle meats such as beef, pork, fowl, and fish. Researchers have identified 17 different HCAs resulting from the cooking of muscle meats that may pose human cancer risk.
In laboratory experiments, HCAs and PAHs have been found to be mutagenic—that is, they cause changes in DNA that may increase the risk of cancer. HCAs are formed when amino acids (the building blocks of proteins), sugars, and creatine (a substance found in muscle) react at high temperatures. PAHs are formed when fat and juices from meat grilled directly over an open fire drip onto the fire, causing flames. These flames contain PAHs that then adhere to the surface of the meat. PAHs can also be formed during other food preparation processes, such as smoking of meats.
Factor influenced in formation of HCA & PHA
The formation of HCAs and PAHs varies by meat type, cooking method, and “doneness” level (rare, medium, or well done). Whatever the type of meat, however, meats cooked at high temperatures, especially above 300ºF (as in grilling or pan frying), or that are cooked for a long time tend to form more HCAs. For example, well done, grilled, or barbecued chicken and steak all have high concentrations of HCAs. Cooking methods that expose meat to smoke or charring contribute to PAH formation. HCAs and PAHs become capable of damaging DNA only after they are metabolized by specific enzymes in the body, a process called “bioactivation.” Studies have found that the activity of these enzymes, which can differ among people, may be relevant to cancer risks associated with exposure to these compounds.
Ongoing studies regards meat intake, cooking methods & cancer risk
Researchers in the United States are currently investigating the association between meat intake, meat cooking methods, and cancer risk. Ongoing studies include the NIH-AARP Diet and Health Study, the American Cancer Society’s Cancer Prevention Study II, the Multiethnic Cohort, and studies from Harvard University. Similar research in a European population is being conducted in the European Prospective Investigation into Cancer and Nutrition (EPIC) study.
Hope new information(s) will be available by the above investigations.
Important information about atorvastatin
You should not take atorvastatin if you are allergic to it, if you are pregnant or breast-feeding, or if you have liver disease. Stop taking atorvastatin and tell your pharmacist right away if you become pregnant. Before taking atorvastatin, tell your pharmacist if you have a thyroid disorder, muscle pain or weakness, a history of liver or kidney disease, or if you drink more than 2 alcoholic beverages daily. In rare cases, atorvastatin can cause a condition that results in the breakdown of skeletal muscle tissue, leading to kidney failure. Call your pharmacist right away if you have unexplained muscle pain, tenderness, or weakness especially if you also have fever, unusual tiredness, and dark colored urine. Avoid eating foods that are high in fat or cholesterol. Atorvastatin will not be as effective in lowering your cholesterol if you do not follow a cholesterol-lowering diet plan. Avoid drinking alcohol. It can raise triglyceride levels and may increase your risk of liver damage. There are many other drugs that can increase your risk of serious medical problems if you take them together with atorvastatin. Tell your pharmacist about all medications you use. This includes prescription, over-the-counter, vitamin, and herbal products. Do not start a new medication without telling your pharmacist. Keep a list of all your medicines and show it to any healthcare provider who treats you. Atorvastatin is only part of a complete program of treatment that also includes diet, exercise, and weight control. Follow your diet, medication, and exercise routines very closely.
Pharmacodynamics
Atorvastatin, a selective, competitive HMG-CoA reductase inhibitor, is used to lower serum total and LDL cholesterol, apoB, and triglyceride levels while increasing HDL cholesterol. High LDL-C, low HDL-C and high TG concentrations in the plasma are associated with increased risk of atherosclerosis and cardiovascular disease. The total cholesterol to HDL-C ratio is a strong predictor of coronary artery disease and high ratios are associated with higher risk of disease. Increased levels of HDL-C are associated with lower cardiovascular risk. By decreasing LDL-C and TG and increasing HDL-C, atorvastatin reduces the risk of cardiovascular morbidity and mortality. Atorvastatin has a unique structure, long half-life, and hepatic selectivity, explaining its greater LDL-lowering potency compared to other HMG-CoA reductase inhibitors.
Mechanism of action
Atorvastatin selectively and competitively inhibits the hepatic enzyme HMG-CoA reductase. As HMG-CoA reductase is responsible for converting HMG-CoA to mevalonate in the cholesterol biosynthesis pathway, this results in a subsequent decrease in hepatic cholesterol levels. Decreased hepatic cholesterol levels stimulates upregulation of hepatic LDL-C receptors which increases hepatic uptake of LDL-C and reduces serum LDL-C concentrations.
Prescribed For
Atorvastatin is used for the treatment of elevated total cholesterol, LDL, and triglycerides and to elevate HDL cholesterol. The effectiveness of atorvastatin in lowering cholesterol is dose-related, meaning that higher doses reduce cholesterol more. Atorvastatin prevents angina, stroke, heart attack, hospitalization for congestive heart failure, and revascularization procedures in individuals with coronary artery disease. Atorvastatin reduces the risk of myocardial infarction (heart attack), stroke, angina and revascularization procedures in adults with multiple risk factors for coronary artery disease. Atorvastatin also prevents heart attacks and strokes in patients with type 2 diabetes with multiple risk factors for coronary artery disease.
Dosage & Administration
Atorvastatin is prescribed once daily. The usual starting dose is 10-20 mg per day, and the maximum dose is 80 mg per day. Individuals who need more than a 45% reduction in LDL cholesterol may be started at 40 mg daily. Atorvastatin may be taken with or without food and at any time of day.
Atorvastatin Breastfeeding Warnings There are no data on the excretion of atorvastatin into human milk; however, a small amount of another drug in this class does pass into breast milk. Atorvastatin is contraindicated in nursing women. The manufacturer recommends that due to the potential for serious adverse reactions in nursing infants, it is recommended that mothers discontinue nursing prior to initiation of therapy with atorvastatin.
Based on animal data, atorvastatin is likely to be excreted into human milk. Nursing animal pups of mothers administered atorvastatin had plasma and liver drug levels 50% and 40%, respectively, of that of their mother's milk. Animal breast milk drug levels may not accurately reflect human breast milk levels.
Drug Interactions
Decreased elimination of atorvastatin could increase levels of atorvastatin in the body and increase the risk of muscle toxicity from atorvastatin. Therefore, atorvastatin should not be combined with drugs that decrease its elimination. Examples of such drugs include erythromycin , ketoconazole ,itraconazole , clarithromycin , telithromycin , cyclosporine , nefazodone , and HIV protease inhibitors such as indinavir and ritonavir.
Cooked Red Meat – A potential foodstuff that increase cancer risk (Study Revealed)
Cancer
Cancer is a very deleterious disease characterized by abnormal division of cells due to abnormality in cell cycle, resulting an unwanted growth called neoplasm and the process is neoplasia. The cells of neoplasm has no morphological, physiological similarities to normal body cells. Any substance’s which can cause mutation (change in nucleobase sequences) are referred as “Carcinogens/ Mutagens”. In every cancer types, mutation is the way which leads the cell to metastasis.
Red Meat
Red meat in traditional culinary terminology is meat which is red when raw and not white when cooked. Red meat also includes the meat of most adult mammals. Cooked Red Meat is now a very popular foodstuff worldwide. Processed Red Meat like fried, grilled, broiled meat are too much delicious meal for most of the peoples worldwide.
Chemicals in Cooked Red Meat
Some recent research shown that, cooked meat at high temperature create chemicals that are not present in uncooked meat. Some of the chemicals can increase cancer risk. The chemicals produced in cooked meat are namely- Heterocyclic amines (HCAs), Polycyclic Aromatic Hydrocarbons (PAHs). Research conducted by the National Cancer Institute (NCI) as well as by Japanese and European scientists indicates that heterocyclic amines are created within muscle meats during most types of high temperature cooking. Heterocyclic amines (HCAs) are the carcinogenic chemicals formed from the cooking of muscle meats such as beef, pork, fowl, and fish. Researchers have identified 17 different HCAs resulting from the cooking of muscle meats that may pose human cancer risk.
In laboratory experiments, HCAs and PAHs have been found to be mutagenic—that is, they cause changes in DNA that may increase the risk of cancer. HCAs are formed when amino acids (the building blocks of proteins), sugars, and creatine (a substance found in muscle) react at high temperatures. PAHs are formed when fat and juices from meat grilled directly over an open fire drip onto the fire, causing flames. These flames contain PAHs that then adhere to the surface of the meat. PAHs can also be formed during other food preparation processes, such as smoking of meats.
Factor influenced in formation of HCA & PHA
The formation of HCAs and PAHs varies by meat type, cooking method, and “doneness” level (rare, medium, or well done). Whatever the type of meat, however, meats cooked at high temperatures, especially above 300ºF (as in grilling or pan frying), or that are cooked for a long time tend to form more HCAs. For example, well done, grilled, or barbecued chicken and steak all have high concentrations of HCAs. Cooking methods that expose meat to smoke or charring contribute to PAH formation. HCAs and PAHs become capable of damaging DNA only after they are metabolized by specific enzymes in the body, a process called “bioactivation.” Studies have found that the activity of these enzymes, which can differ among people, may be relevant to cancer risks associated with exposure to these compounds.
Ongoing studies regards meat intake, cooking methods & cancer risk
Researchers in the United States are currently investigating the association between meat intake, meat cooking methods, and cancer risk. Ongoing studies include the NIH-AARP Diet and Health Study, the American Cancer Society’s Cancer Prevention Study II, the Multiethnic Cohort, and studies from Harvard University. Similar research in a European population is being conducted in the European Prospective Investigation into Cancer and Nutrition (EPIC) study.
Hope new information(s) will be available by the above investigations.
PARACETAMOL (ACETAMINOPHEN) & HEPATOTOXICITY
Paracetamol is widely available and has been around since the 1950s. It is widely prescribed and cheap to buy over-the-counter (Without any prescriptions), making it a common drug taken in overdose. It is a very useful analgesic (Pain Killer) (alone or in combination) and also is an antipyretic(Fever reducer) . It is normally found as a 500 mg tablet, but it is often combined with other active ingredients in various preparations. Paracetamol is used to treat many conditions such as headache, muscle aches, arthritis, backache, toothaches, colds, and fevers. It relieves pain in mild arthritis but has no effect on the underlying inflammation and swelling of the joint. Paracetamol may also be used for other purposes not listed in this medication guide.
Important information about paracetamol
There are many brands and forms of paracetamol available. Do not use more of this medication than is recommended. An overdose of paracetamol can cause serious harm. The maximum amount of paracetamol for adults is 1 gram (1000 mg) per dose and 4 grams (4000 mg) per day. Taking more paracetamol could cause damage to your liver. If you drink more than three alcoholic beverages per day, talk to your pharmacist or doctor before taking paracetamol and never use more than 2 grams (2000 mg) per day. Do not use this medication without first talking to your pharmacist or doctor if you drink more than three alcoholic beverages per day or if you have had alcoholic liver disease (cirrhosis). You may not be able to use paracetamol. Before using paracetamol , tell your doctor if you have liver disease or a history of alcoholism.
Do not use any other over-the-counter cough, cold, allergy, or pain medication without first asking your doctor or pharmacist. Paracetamol is contained in many combination medicines. If you use certain products together you may accidentally use too much paracetamol . Read the label of any other medicine you are using to see if it contains paracetamol, acetaminophen . Avoid drinking alcohol while taking this medication. Alcohol may increase your risk of liver damage while taking paracetamol .
Pathophysiology of Hepatotoxicity by Paracetamol (At overdose)
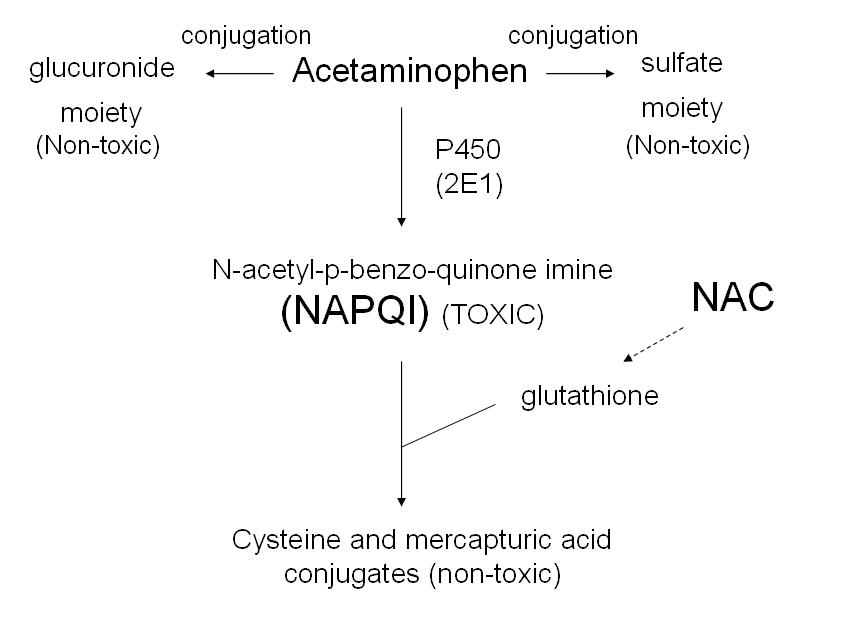
After taken orally, paracetamol is well absorbed from the stomach and small intestine and reaches a peak plasma concentration in one hour. It is inactivated by the liver by conjugation leading to two metabolites- glucoronide or sulfate. It is then excreted(leave the body) through urine.
-When taken in overdose the liver conjugation becomes inundated, causing paracetamol to be metabolised by an alternative pathway.
-This results in a toxic metabolite, N-acetyl-p-benzoquinone imine (NABQI), which is itself inactivated by glutathione, rapidly preventing any harm.
-However, glutathione can be run down with minor increases in the toxin and, when this occurs, NABQI reacts with nucleophilic aspects of the cell, leading to necrosis. Necrosis occurs in the liver and in the kidney tubules.
Paracetamol is widely available and has been around since the 1950s. It is widely prescribed and cheap to buy over-the-counter (Without any prescriptions), making it a common drug taken in overdose. It is a very useful analgesic (Pain Killer) (alone or in combination) and also is an antipyretic(Fever reducer) . It is normally found as a 500 mg tablet, but it is often combined with other active ingredients in various preparations. Paracetamol is used to treat many conditions such as headache, muscle aches, arthritis, backache, toothaches, colds, and fevers. It relieves pain in mild arthritis but has no effect on the underlying inflammation and swelling of the joint. Paracetamol may also be used for other purposes not listed in this medication guide.
Important information about paracetamol
There are many brands and forms of paracetamol available. Do not use more of this medication than is recommended. An overdose of paracetamol can cause serious harm. The maximum amount of paracetamol for adults is 1 gram (1000 mg) per dose and 4 grams (4000 mg) per day. Taking more paracetamol could cause damage to your liver. If you drink more than three alcoholic beverages per day, talk to your pharmacist or doctor before taking paracetamol and never use more than 2 grams (2000 mg) per day. Do not use this medication without first talking to your pharmacist or doctor if you drink more than three alcoholic beverages per day or if you have had alcoholic liver disease (cirrhosis). You may not be able to use paracetamol. Before using paracetamol , tell your doctor if you have liver disease or a history of alcoholism.
Do not use any other over-the-counter cough, cold, allergy, or pain medication without first asking your doctor or pharmacist. Paracetamol is contained in many combination medicines. If you use certain products together you may accidentally use too much paracetamol . Read the label of any other medicine you are using to see if it contains paracetamol, acetaminophen . Avoid drinking alcohol while taking this medication. Alcohol may increase your risk of liver damage while taking paracetamol .
Pathophysiology of Hepatotoxicity by Paracetamol (At overdose)
After taken orally, paracetamol is well absorbed from the stomach and small intestine and reaches a peak plasma concentration in one hour. It is inactivated by the liver by conjugation leading to two metabolites- glucoronide or sulfate. It is then excreted(leave the body) through urine.
-When taken in overdose the liver conjugation becomes inundated, causing paracetamol to be metabolised by an alternative pathway.
-This results in a toxic metabolite, N-acetyl-p-benzoquinone imine (NABQI), which is itself inactivated by glutathione, rapidly preventing any harm.
-However, glutathione can be run down with minor increases in the toxin and, when this occurs, NABQI reacts with nucleophilic aspects of the cell, leading to necrosis. Necrosis occurs in the liver and in the kidney tubules.
Toxicity is increased in patients with induction of the P450 system through drugs such as rifampicin, phenobarbital, phenytoin, carbamazepine and alcohol. This also occurs in patients with low glutathione reserves, as a product of:
Genetic variation
HIV positive
Malnutrition
Alcohol-related or other liver disease
Paediatric patients (under the age of 5 years) seem to fare better after paracetamol poisoning, perhaps due to a greater capacity to conjugate with sulfate, enhanced detoxification of NABQI or greater glutathione stores. However, it should not be assumed that treatment in children should be different than for adults, since no controlled studies have supported any alternative paediatric therapy.
SAVE PARACETAMOL, SAVE YOUR LIFE
Genetic variation
HIV positive
Malnutrition
Alcohol-related or other liver disease
Paediatric patients (under the age of 5 years) seem to fare better after paracetamol poisoning, perhaps due to a greater capacity to conjugate with sulfate, enhanced detoxification of NABQI or greater glutathione stores. However, it should not be assumed that treatment in children should be different than for adults, since no controlled studies have supported any alternative paediatric therapy.
SAVE PARACETAMOL, SAVE YOUR LIFE